Objectives:
- Explain robotics as the next progression in surgical history
- Address data-driven risk mitigation
- Review evolution of technology in surgery and SPD
Surgery occupies a distinct place in technological advancement. It is simultaneously one of the oldest professional medical practices and one of the most aggressive in innovation. Throughout the history of surgical innovation, surgery has always been dependent upon tools. As surgical procedures become more complex, minimally invasive medical device complexity increases. This creates a significant challenge for the sterile processing professionals who are charged with cleaning, inspecting, and sterilizing complex medical devices. Consequently, if Sterile Processing is to properly fulfill its role in patient safety, innovations in reprocessing must keep pace with the rate of development in surgery.
Surgical innovation in history
As far back as 6500 B.C, the ancient Egyptians practiced the brutal art of trepanning, drilling holes into the skull to alleviate a number of complaints. Additionally, the Egyptians pioneered another procedure, called couching, to cure cataracts. However, after impressive developments at such an early point in history, surgical innovation stalled for multiple millennia. Surgical procedures were restricted to alleviating a handful of frequent conditions that were often byproducts of an underdeveloped understanding of hygiene. Consequently, surgical instrumentation remained relatively simple.
The rise of the Surgeon/Barber is a great example of the simplicity of surgical instruments and procedures. At that time, 16th century AD, all that was “required” to be a surgeon was a sharp knife and steady hand. Both requirements were readily met by the town barber, who needed a well-maintained knife and steady hand to shave men’s beards. With little training, someone who met these two prerequisites could lance boils and amputate limbs, the two most common surgical procedures of the pre-modern world. Of course, most procedures came with staggering mortality rates. Death from infection after amputation, for example, could be as high as 70% in some cases.[1]Not amputating at all was almost certain death.
The scientific revolution has reshaped almost every aspect of daily life, and medical treatment is no exception. The twin discoveries of antibiotics and steam sterilization enabled surgical procedures and outcomes that would have once seemed impossible. Increasingly complex surgeries gave birth to the development of many of the basic surgical instruments that we still use today. Hemostats, needle-drivers, and self-retaining retractors were at one time considered to be cutting-edge technology, but are now considered the most basic form of surgical instrumentation.
The next major development was the innovation of minimally-invasive surgery (MIS). When compared to other surgical approaches, MIS surgery is still in its infancy. Undoubtedly, there are many individuals serving in the healthcare industry right now who are older than MIS surgery. The rapid adoption of MIS as the preferred approach for many procedures is shocking, given that at the time of its introduction it was described as “a futureless technique”, “circus surgery”, and “a media show of a tightrope dancer who is totally careless of the risks for the patients”.[2] Yet the advantages were so staggering that it quickly overcame the resistance of the surgical status quo.
As with all surgical innovations, the advent of minimally invasive surgery brought with it a host of new instrument designs. However, unique to MIS surgery has been the proliferation of new features that dramatically increase the complexity of instrument design.
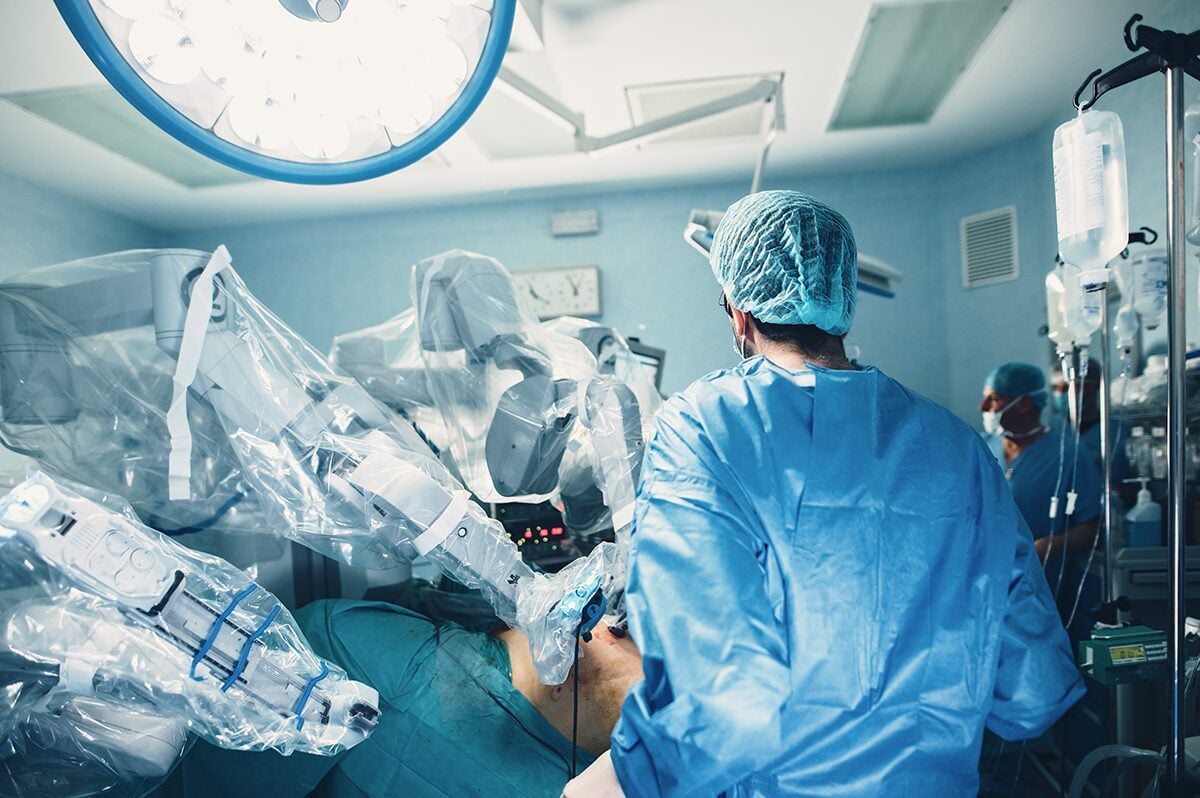
Nowhere is this more apparent than in the advent of robotic surgery, which is still defined as MIS but with added precision and dexterity than traditional laparoscopic instruments simply cannot produce. It is truly an amazing achievement, but we must caution ourselves from believing that “better” means “risk-free”. For example, performing integrity checks and documenting results, such as checking electrosurgical instruments between uses mitigates risk and is also a definable data point that a tracking system should record. Therefore, the role of sterile processing, as the keeper of the tools, must evolve to truly capture the potential of patient benefits while mitigating new risks.
Data-Driven Risk Mitigation
Purchasing decisions
One consistent commonality among all-new complex instruments and devices is a high price tag. Robotic instruments epitomize this perhaps more than any other devices, often costing over $2 million[3] for a new system. It is no surprise that hospitals, which typically run on profit margins of 2-3 percent, seek every opportunity to reduce the extreme expense of investing in new technology. In the case of robotic instruments, a significant portion of the startup costs of a DaVinci System lies in the limited-reuse arms. Sterile processing personnel, who are solely responsible for the cleanliness and functionality of the arms, are all too often the last to be involved (or not involved at all) in the consideration of how many sets of arms should be purchased. The amount of time and resources necessary to ensure the proper care of the arms should figure in to decide how many arms should be purchased. It is also important to note that the correct cleaning equipment must be purchased. For example, depending on the robotic platform purchased will impact what sonics the arms fit in and if the hospital will need to purchase a manifold to fit the sonic or the washer.
Clearly, cost alone cannot be the only consideration for purchasing robotic arms if hospitals are to realize the potential for improved patient outcomes. However, many hospitals lack the tools necessary to make better, data-driven purchasing decisions that can determine if sterile processing is set up for success or failure. Proper use of a tracking system with reliable reporting metrics can be critical for determining the throughput capacity of sterile processing, and therefore, how many arms should be purchased. Too few arms mean more pressure on sterile processing to rush, and frequently cut corners, to meet the OR’s caseload. The excessive stock of lesser-used arms creates waste due to overstocking.
By leveraging all systems involved in your robotic processes, you can have a healthier base for your purchasing decisions. For example, Intuitive Surgical tracks all instruments used during a procedure and provides data to determine inventory. Now combine this data with a tracking system that tracks each time the device is sterilized in order to remain compliant with the manufacturer’s IFU regarding total sterilization cycles permitted.
Compliance
Increasingly complex devices inevitably lead to increasingly complex reprocessing instructions. If sterile processing procedures deviate from the manufacturer’s instructions for use (IFUs) results can be unreliable. A shocking number of hospitals are operating with devices assumed to be sterile simply because the parameters in the autoclave were met. Those parameters offer no guarantees on the condition of the instruments prior to being placed in the autoclave.
It is unreasonable to expect that sterile processing professionals can accurately and reliably memorize every step in every IFU, many of which require dozens of steps to be performed in a specific sequence. By documenting the ultrasonic, washer cycles, and the sterilization cycle, coupled with any cleaning verification testing that can be performed, provides the best assurance. Especially when proper utilization of a tracking system is in place and capturing the aforementioned test. A tracking system is also effective in assisting technicians by guiding them through the IFU and offering assistance, such as pictures or videos, for difficult or complex steps.
Sterilization records are necessary, but they cannot demonstrate compliance with cleaning and function testing prior to the instruments being sterilized. While technology may not yet conclusively demonstrate instrument-level compliance, utilizing a tracking system to document IFUs, videos, and photos provides a massive improvement. Additionally, systems that can restrict the ability of technicians who do not have verified competency to reprocess devices can provide a critical additional layer of quality assurance.
Process Improvement
There is an old business saying: “What gets measured gets improved.” Unsurprisingly, many improvement efforts in sterile processing amount to little more than putting out fires, often because of the lack of actionable data. Proper utilization of data reporting can be used to identify trends in usage, delays, and throughput (as mentioned previously). Gathering such data would be almost impossible without a tracking system. However, collecting data and properly interpreting it are two very different things. While the number of facilities utilizing a tracking system is growing, there is still much room for improvement when it comes to using those tracking systems to their fullest potential. Too many sterile processing departments treat their tracking system as a fancy count sheet printer. Many sterile processing managers find themselves overwhelmed at the amount of raw data that a tracking system may make available because they lack the training and tools to make the data meaningful for decision-making. A critical opportunity exists for on-going data analytic and process improvement training for tracking system customers. Once managers are empowered to understand reports, identify opportunities for improvement, and document their efforts, SPD leadership may finally see the increasing support that they have been desperately wanting from administrators.
Conclusion
Surgery, by its nature, will always seek the next step in improving patient outcomes. However, decision-makers should be mindful that the pace of technological advancement can easily exceed the pace of our understanding of risk and how to mitigate that risk. Many of the tools necessary to meet the reprocessing challenges posed by robotic instruments already exist. In the case of data, the trouble in many facilities is not gathering data but understanding how to apply it. Without concerted efforts and partnerships between vendors and healthcare facilities to implement and train on the most effective use of information, the potential for improvements to patient care will never be fully realized.
Take the Quiz to Receive Your CE Credits!