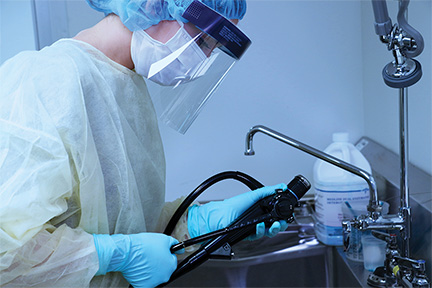
In April 2015, the Association for the Advancement of Medical Instrumentation released AAMI ST 91 which covers the entire gamut of information for reprocessing endoscopes from room design to having qualified and competent staff reprocessing these delicate, costly, and complex medical devices. If you don’t already have a copy of AAMI ST 91, it is imperative that you obtain a copy for either yourself or your facility (Purchase a Copy).
Back in 2011, the Multisociety Guidelines on Reprocessing Flexible Gastrointestinal Endoscopes was published to address the same issues through an interdisciplinary group. And actually, the standard being discussed here started out to be a TIR (Technical Information Report), a less formal document than a standard. The AAMI Endoscope Reprocessing Group determined, however, that more specific and formal guidance was needed to address the issues. This resulted in our current AAMI standard released in April 2015. For the SPD Manager or the Manager of an Endoscopy suite, this document is a “must have” in your library of resources.
In the following paragraphs, we will focus on what the need-to-know aspects of scope reprocessing are. The information corresponds to sections five (5) and twelve (12) of the AAMI ST 91.
List of Tasks
Section 5 includes what AAMI refers to as a comprehensive list of tasks required for proper cleaning and high level disinfection (HLD). We’ll list them in summary but will provide some commentary for each as we move through the discussion. Please keep in mind that one is not more or less important than the others. All steps identified are critical to providing a safe medical device to be used on your next patient. The steps referred to are:
- Precleaning at the point of use (POU)
- Transportation
- Leak testing
- Cleaning
- Rinsing
- Inspection
- HLD and monitoring of the process
- Rinsing
- Drying and alcohol flush
- Storage
POU Cleaning
Whether it seems to be a feasible approach or not, both AORN and AAMI have always recommended POU cleaning. This is especially essential in consideration of our flexible endoscopes. If this isn’t completed immediately after the endoscopic procedure, bioburden remains on the surfaces of the scope, biofilms are given an invitation to form on the scope’s surfaces, and body secretions that came in contact with the device are permitted to dry on the device. All of these negative effects not only are a compromise to the recommended practices, but the effective removal of the above has just become much more difficult to properly clean the device prior to the HLD process. Critical steps such wiping down the insertion tube, suction cleaning solutions through the working channels, and ensuring that the channels aren’t blocked are critical to the successful reprocessing of a scope.
Transportation
Each endoscope that has been used for a medical procedure should be safely transported from the patient procedure room to the decontamination and reprocessing area. Used scopes need to be contained during transport and all the accessory equipment for the scope should be kept together and delivered together. Everything should go through the steps for reprocessing as a unit, but with multiple parts.
Leak Testing
Not all manufacturers and models of flexible endoscopes may require the device to be leak tested. We must be diligent in determining which types require the special testing as well as ensure that personnel responsible for handling these devices are adequately informed and knowledgeable of the specific requirements for every model being processed. Proper and timely leak testing is critical to the preservation of these complex devices. Leak testing will produce evidence that the endoscope is functional and if immersed in cleaning solutions or disinfectant solutions, the device will not be damaged as a result of fluid invasion. There are many methods for effective leak testing and can be either a manual or automated process. Regardless, departments must be aware of each and what is the expected protocol of the facility. (See AAMI ST 91, 5.4 for descriptions of leak tests.)
Manual Cleaning
Just as POU precleaning can’t be overlooked in our reprocessing steps, neither can the manual cleaning of each of our flexible endoscopes. It’s a well known and familiar adage that, “if it isn’t clean, it can’t be sterilized”. Likewise “if it isn’t clean, it can’t be High Level Disinfected.” Bioburden remaining on the device and biofilms having formed on the device and not properly removed and eradicated before disinfection will prevent effective HLD. Fresh enzyme (or other cleaning solutions) must be prepared for every scope being reprocessed to avoid cross contamination.
Manual Rinsing
Thorough rinsing is no less important than any other step listed here. After the endoscope has been cleaned, it is important to remove any chemical residual remaining on outside surfaces, valves, and channels. After cleaning and rinsing, keep all accessory parts together with the scope and treat it as a complete unit.
Inspection
Inspection of the endoscope should not just be a once and done action. Through each stage of the reprocessing, it is prudent for the technician to do a visual inspection, ensuring there is no visible debris or damage on the endoscope and taking the appropriate action for any findings.
High Level Disinfection (HLD)
HLD can be an automated or a manual process. Both practices are acceptable and related documentation is critical for either method. See your manufacturer’s instructions for use for details either way. In either method, attention to detail must be given to the effectiveness of the disinfection solution, no topping off solutions, performing an MEC/MRC (minimum effective concentration/minimum required concentration) test strip, the required length of time the devices needs to be exposed to the HLD, and to ensure that all the HLD solution and residuals are thoroughly rinsed from the device.
Rinsing
If your department has an AER (Automated Endoscope Reprocesser), rinsing the device will be performed in the equipment itself and the parameters that are required are automatically recorded at the time of the cycle. If manual rinsing is performed, strict adherence must be practiced to use copious amounts of some type of purified water for the final rinse of the device.
Alcohol Flush
Flexible endoscopes have an incredibly high number of areas that if left uncared for, will definitely present potential situations for patient safety. It is therefore recommended that all channels on the device are flushed with alcohol and dried. (Again, check with the manufacturer’s IFU). Once the endoscope is thoroughly and properly cleaned and HLD, it becomes necessary to preserve the clean surfaces for subsequent use. Alcohol, being a disinfectant in its own properties is also used for the rapid evaporation. The alcohol will expedite proper drying of those parts we cannot visualize. The scope needs to remain dry from this point on or the potential for growth of bacteria increases.
Storage
Endoscopes should be stored in a dedicated, closed, ventilated cabinet. The scopes should be hung in order to have all channels hanging vertically, so if there is potential moisture remaining, it will drain out by gravity. Each facility must determine the expiration date or “hang time” that the scopes are able to remain in the cabinets before being reprocessed. There are no definitive guidelines regarding hang time, it is up to the facility to review all the appropriate studies that have been made available and adopt that which works best for the facility.
The other specific section of AAMI ST 91 that needs to be carefully considered is section twelve, dealing comprehensively with Quality Control. Some of the critical points to consider are product identification and traceability, documentation and recordkeeping, cleaning verification, and labeling. Recordkeeping for endoscopes is just as important for the endoscopes as it is for the items brought to our SPDs for terminal sterilization. The rigors and types of information required to be documented are vast, and it is important that we are able to maintain all aspects for the endoscope requirements.
While there may be multiple stringencies and guidelines for effective scope reprocessing, it is up to all of us to ensure that our facilities are following best practices and ensuring paramount care for our patients, wherever they have these procedures performed.